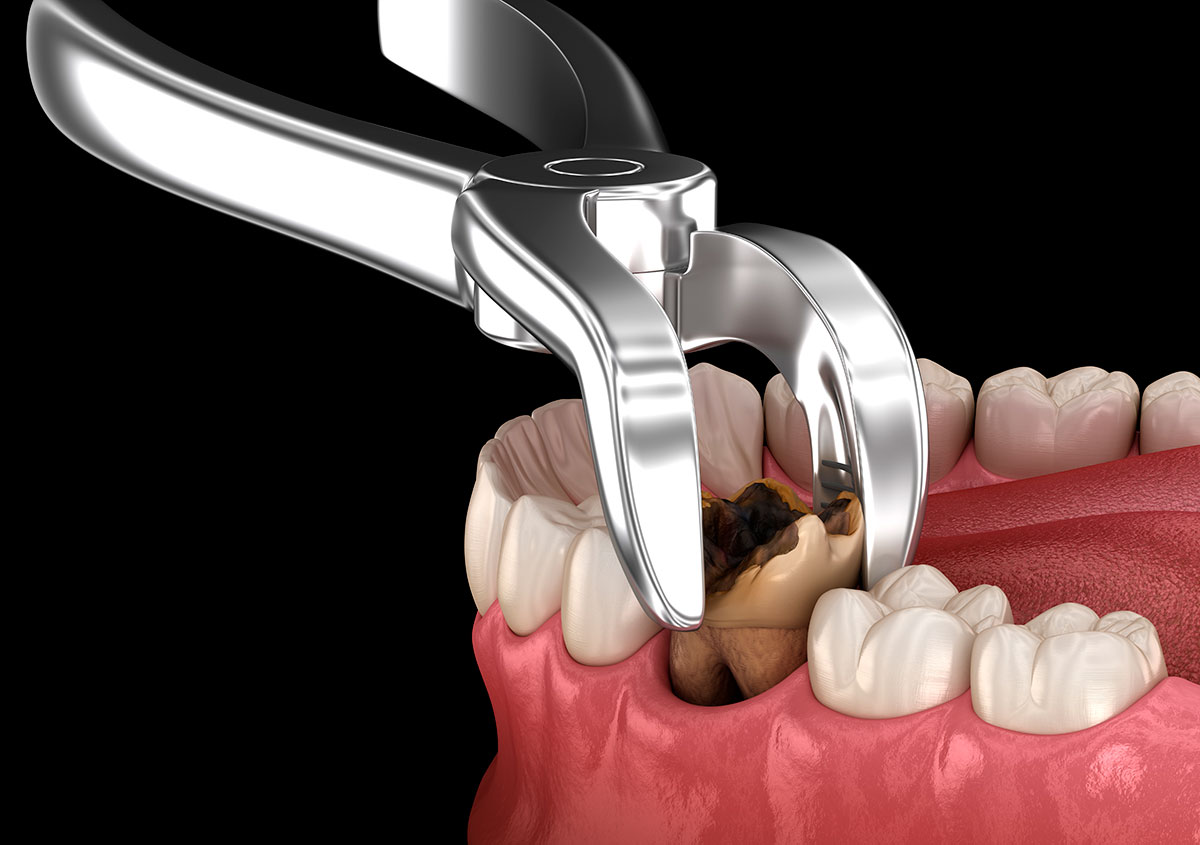
Oral surgery is often perceived as simple, yet a Tooth Extraction can sometimes become unexpectedly complex when roots are curved, bone is dense, or infection has altered the surrounding tissues. In these situations, what appears to be a routine Tooth Extraction may turn into a challenging surgical procedure that influences the jawbone, nerves, and overall oral balance. Understanding how a difficult Tooth Extraction interacts with jaw and oral health helps patients make informed decisions while appreciating the biological complexity behind every removal.
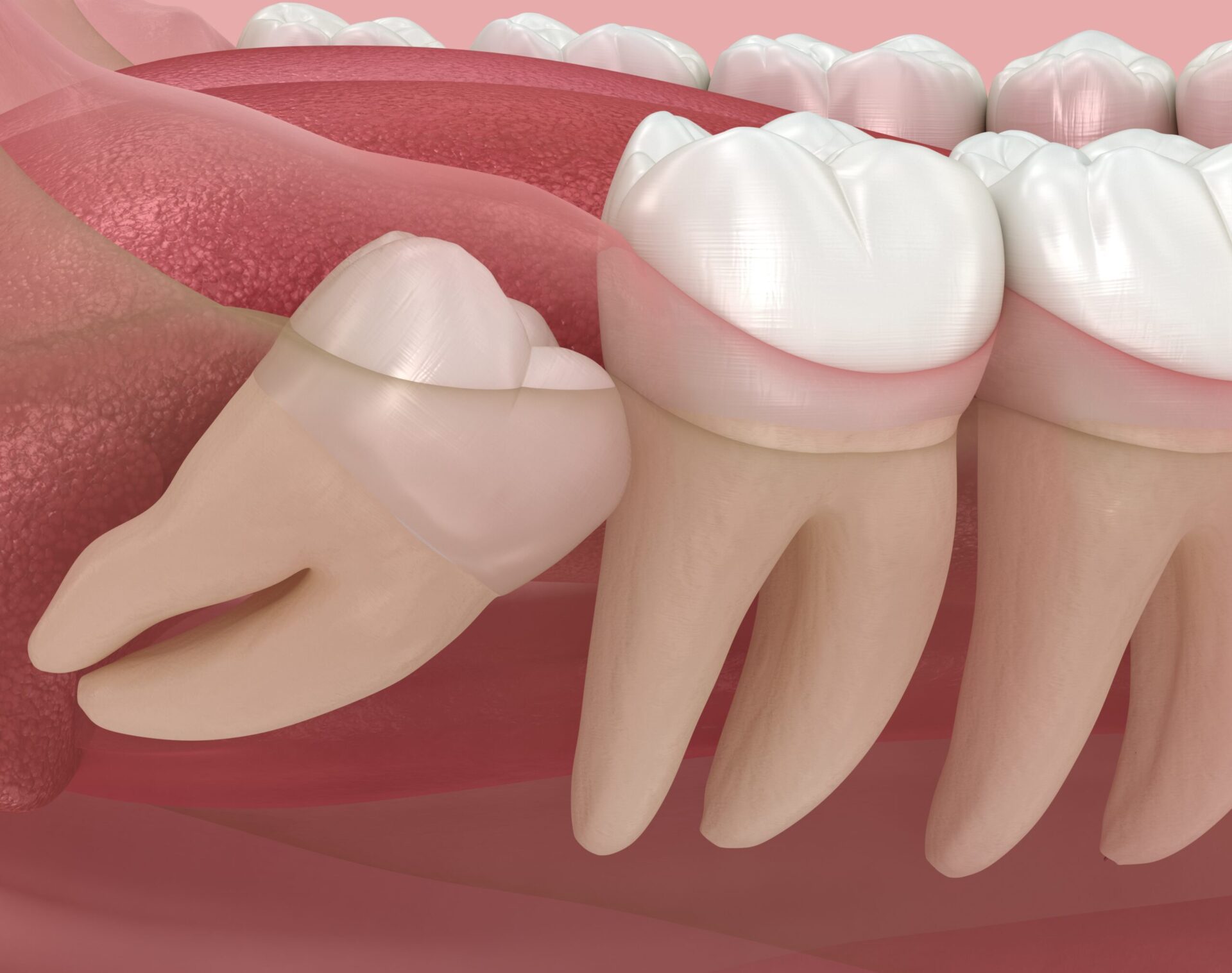
These observations highlight that each Tooth Extraction interacts with biology in measurable yet manageable ways.

What Makes a Tooth Extraction Difficult?
A standard Tooth Extraction usually involves loosening the tooth and lifting it from the socket with minimal resistance. However, difficulty increases when anatomical or pathological factors interfere with access or visibility. Impacted wisdom teeth, deeply fractured roots, and teeth fused to bone through ankylosis can complicate the procedure. In such cases, a surgical Tooth Extraction may require bone removal, tooth sectioning, or delicate flap design. Each added step lengthens the procedure and increases tissue manipulation. Research in oral surgery literature suggests that bone density, patient age, and chronic inflammation play significant roles. Dense cortical bone can resist instruments, while inflamed tissues bleed more easily. These variables transform a simple Tooth Extraction into a more technical intervention that demands precision and planning.How a Tooth Extraction Influences Jawbone Structure
The jawbone is a living tissue that adapts to mechanical forces. When a tooth is present, chewing stimulates the surrounding bone, preserving its volume. After a Tooth Extraction, that stimulation decreases. Within the first few months following a Tooth Extraction, the body naturally remodels the empty socket. Studies show that some degree of bone resorption may occur. This does not necessarily indicate damage, but rather the bone adapting to reduced function. Still, noticeable changes in width and height may affect neighboring teeth. From a biomechanical perspective, multiple Tooth Extraction procedures over time can influence bite alignment. Reduced bone support may shift load distribution, which sometimes alters chewing patterns. For this reason, clinicians often evaluate long term restorative plans after a surgical Tooth Extraction.Soft Tissue Healing After Tooth Extraction
Healing of the gums is just as important as bone recovery. After a Tooth Extraction, a blood clot forms inside the socket. This clot protects deeper tissues and serves as a scaffold for new cells. When the clot remains stable, epithelial tissue gradually covers the area. However, disruption of the clot may delay healing. A complicated Tooth Extraction involving incisions or sutures typically requires more time for the gum margin to normalize. Soft tissue responses vary between individuals. Factors such as oral hygiene, smoking habits, and immune response can influence the healing timeline after a Tooth Extraction. Observing the biological sequence helps explain why some people recover faster than others.Nerve and Sinus Considerations in Surgical Tooth Extraction
Certain teeth lie close to important anatomical structures. Lower molars may be near the inferior alveolar nerve, while upper molars can be close to the maxillary sinus. During a complex Tooth Extraction, these relationships matter greatly. Advanced imaging often helps clinicians evaluate proximity before performing a Tooth Extraction. Temporary sensations such as tingling or numbness sometimes occur when tissues are manipulated. These effects are usually transient and related to inflammation rather than permanent injury. In upper posterior regions, the sinus floor may be thin. A surgical Tooth Extraction in this area sometimes requires extra care to avoid sinus communication. Understanding this anatomy highlights why not every Tooth Extraction is identical, even when symptoms seem similar.
Functional Changes After Tooth Extraction in Daily Life
Teeth work as a coordinated system. Removing one tooth through Tooth Extraction can subtly influence chewing efficiency and bite balance. Adjacent teeth may drift into the space, and opposing teeth may slightly over erupt. These changes do not occur immediately, but over months or years. Following a Tooth Extraction, the masticatory system gradually redistributes forces. Some patients notice minor differences in pressure or chewing rhythm. Speech articulation and facial support can also shift depending on the tooth’s location. Although most adjustments are small, awareness of these functional adaptations helps explain why dentists sometimes discuss restorative options after a Tooth Extraction rather than viewing the procedure as an isolated event.Scientific Insights Into Risks and Outcomes of Tooth Extraction
Clinical studies often categorize complications into short term and long term outcomes. Short term issues may include swelling, mild bleeding, or limited mouth opening after a Tooth Extraction. These are usually part of normal inflammatory processes. Long term observations focus on bone remodeling and neighboring tooth stability. Data from oral surgery reports indicate that well planned Tooth Extraction procedures generally show predictable healing patterns. Complications tend to be associated with infection, systemic conditions, or complex anatomy rather than the act of extraction itself. Below is a simplified overview of commonly discussed outcomes:| Factor | Possible Effect After Tooth Extraction | Typical Course |
| Bone remodeling | Reduced socket volume | Gradual adaptation |
| Soft tissue healing | Temporary swelling | Resolves over time |
| Bite changes | Minor shifting | Slow progression |
| Sensory response | Temporary tingling | Often short lived |
Planning Around a Tooth Extraction for Long Term Oral Health
A thoughtful approach often begins before the Tooth Extraction itself. Radiographs, digital scans, and clinical evaluations guide the surgical strategy. Anticipating bone shape and root orientation reduces unnecessary trauma. After a Tooth Extraction, many clinicians consider preservation techniques such as socket management or future restorative planning. These concepts aim to maintain oral harmony rather than simply removing the tooth and moving on. At ClinicHI, the philosophy centers on viewing every Tooth Extraction as part of a broader oral ecosystem. By integrating surgical knowledge with restorative thinking, the goal is to support stable outcomes that respect both function and aesthetics. A difficult Tooth Extraction is more than a mechanical procedure. It is a biological event that interacts with bone, gums, nerves, and overall oral dynamics. From the initial surgical steps to the subtle remodeling that follows, each Tooth Extraction leaves a measurable imprint on the jaw and surrounding tissues. When examined through a scientific lens, these changes are not alarming but adaptive. The human body continuously reorganizes itself to maintain balance. Understanding this process transforms the idea of Tooth Extraction from a simple removal into a carefully orchestrated phase of oral health management. By exploring the structural, functional, and anatomical effects together, patients gain a clearer perspective on what truly happens during and after a Tooth Extraction, and why precision, planning, and expertise matter in every case.Get Your Free Consultation
Have questions? Leave your details and we'll get back to you as soon as possible.
Get Free Consultation