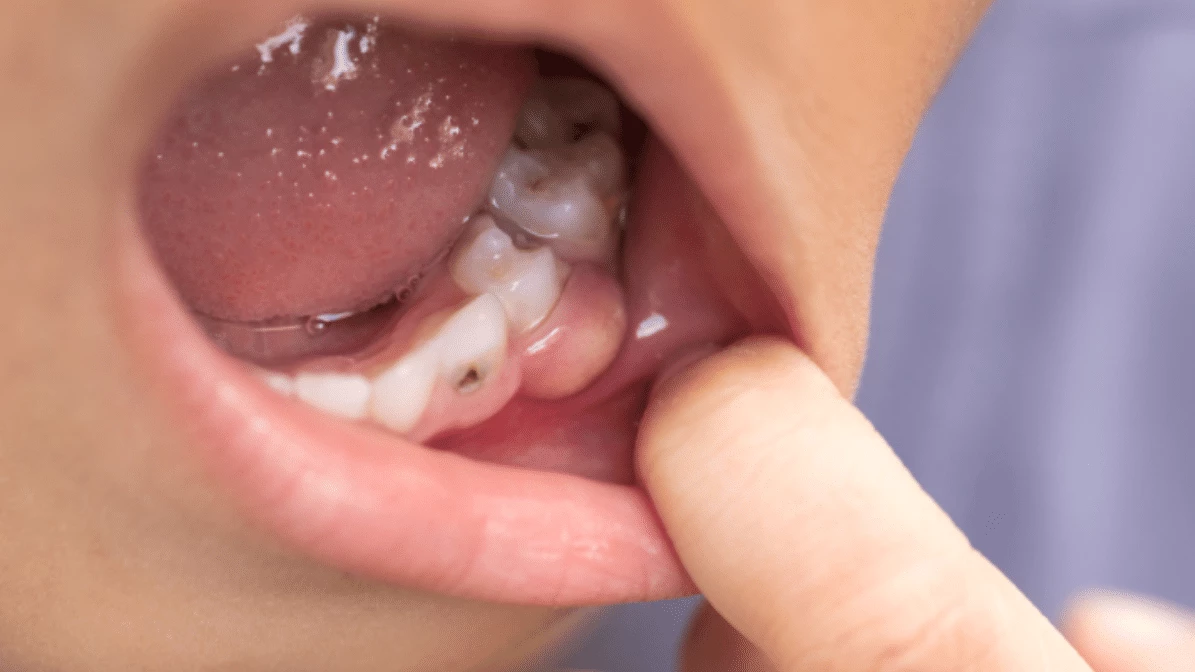
Dental Infections are among the most commonly discussed topics in modern oral health, not only in clinics but also in scientific literature and public health research. From localized tooth abscesses to more complex oral bacterial conditions, Dental Infections raise important questions about treatment approaches, antibiotic resistance, and long term outcomes. For patients and professionals alike, understanding how antibiotics relate to Dental Infections has become a critical part of contemporary dental awareness.
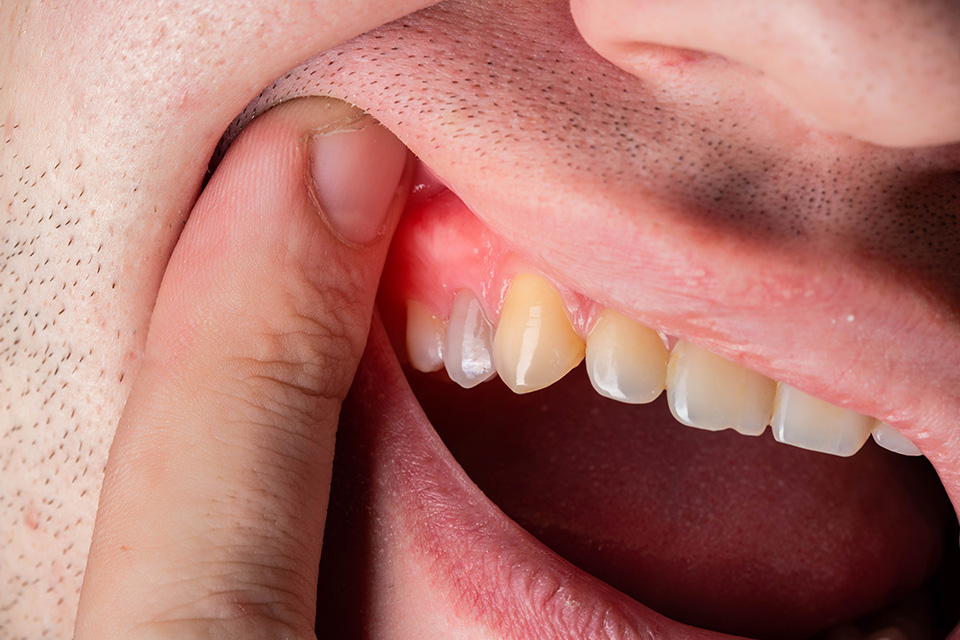
Scientific literature emphasizes that not all Dental Infections behave the same way. Some remain localized, while others show patterns of spread. Antibiotics are more frequently associated with discussions of Dental Infections that extend beyond the tooth structure itself.

Understanding Dental Infections and Oral Bacteria
Dental Infections originate when oral bacteria penetrate deeper tooth structures or surrounding tissues. This process often begins with enamel damage, untreated decay, or gum inflammation, creating an environment where bacteria thrive. Scientific studies show that Dental Infections are rarely caused by a single microorganism, but rather by complex bacterial communities. From a microbiological perspective, Dental Infections involve aerobic and anaerobic bacteria working together. These bacterial ecosystems explain why some Dental Infections progress slowly while others escalate rapidly. Researchers emphasize that antibiotics interact differently with these bacterial groups, which affects how Dental Infections respond to medication. Another important factor is the body’s immune response. In many Dental Infections, inflammation and swelling are driven as much by immune activity as by bacteria themselves. This is why antibiotics alone may not fully resolve Dental Infections, a point highlighted in multiple dental research reviews.How Antibiotics Interact With Dental Infections
Antibiotics target bacteria, not the structural cause of Dental Infections. This distinction is central to understanding their role. In clinical discussions, antibiotics are often described as supportive tools rather than primary solutions for Dental Infections. When prescribed, antibiotics may reduce bacterial load associated with Dental Infections, potentially limiting spread to surrounding tissues. However, studies indicate that antibiotics do not remove infected tissue or repair damaged teeth. This explains why mechanical or procedural interventions remain central in managing Dental Infections. Another layer involves antibiotic spectrum. Broad spectrum antibiotics may affect multiple bacterial strains linked to Dental Infections, while narrow spectrum options target specific bacteria. Research comparing these approaches suggests that indiscriminate use may disrupt normal oral flora, indirectly influencing future Dental Infections.Antibiotic Resistance and Dental Infections
One of the most researched topics today is antibiotic resistance in relation to Dental Infections. Global health reports consistently identify dental antibiotic use as a contributor to resistance trends. This does not mean antibiotics are ineffective, but it highlights the complexity of treating Dental Infections responsibly. Repeated exposure to antibiotics can allow bacteria associated with Dental Infections to adapt. Resistant strains may survive treatment and become harder to manage in future infections. This phenomenon has been documented in both hospital and community dental settings. Interestingly, some studies suggest that resistance linked to Dental Infections develops faster when antibiotics are used without clear bacterial spread. These findings have reshaped how professionals think about prescribing patterns related to Dental Infections, emphasizing caution and precision.Common Types of Dental Infections Discussed in Research
Different categories of Dental Infections respond differently to antibiotics. Understanding these distinctions helps clarify why antibiotics are sometimes used and sometimes avoided.| Type of Dental Infection | Primary Characteristics | Antibiotic Relevance |
| Periapical Infection | Originates at tooth root | Often adjunctive |
| Periodontal Infection | Affects gum and bone | Case dependent |
| Pericoronitis | Around partially erupted teeth | Situational |
| Facial Space Infection | Spreads beyond oral cavity | More commonly discussed |
Myths and Misconceptions About Dental Infections
Public perception of Dental Infections often includes the assumption that antibiotics are always necessary. Surveys show that many patients expect antibiotics as a default response to Dental Infections, even in cases where evidence does not support this approach. Another misconception is that antibiotics cure Dental Infections permanently. Research repeatedly clarifies that antibiotics may temporarily suppress symptoms but do not eliminate the underlying cause. This misunderstanding has fueled unnecessary antibiotic demand related to Dental Infections worldwide. There is also confusion about pain and infection. Not all dental pain indicates Dental Infections, and not all Dental Infections cause immediate pain. These nuances highlight why education around Dental Infections is as important as treatment discussions.
Scientific Perspectives on Managing Dental Infections
Modern dentistry approaches Dental Infections through multidisciplinary analysis. Epidemiological studies, microbiology research, and clinical observations all contribute to evolving perspectives. Antibiotics are now viewed as one component within a broader management framework for Dental Infections. Research from academic dental journals emphasizes early detection and localized intervention. By addressing Dental Infections at their source, reliance on antibiotics may be reduced. This approach aligns with global efforts to slow antibiotic resistance. Another emerging topic involves patient specific factors. Age, immune status, and systemic conditions influence how Dental Infections behave and how antibiotics interact with them. These insights reinforce the idea that Dental Infections cannot be approached with a one size fits all mindset.The Future of Antibiotics in Dental Infections
Looking ahead, the role of antibiotics in Dental Infections continues to evolve. Ongoing studies explore targeted antimicrobial agents, improved diagnostics, and alternative strategies that complement traditional approaches to Dental Infections. Artificial intelligence and microbiome analysis are also shaping future conversations. These technologies may help identify which Dental Infections truly benefit from antibiotics and which do not. Such advancements aim to balance effective care with responsible antibiotic use. For institutions like ClinicHI, staying aligned with current research ensures that discussions around Dental Infections remain informed, balanced, and forward thinking. As science advances, understanding antibiotics in the context of Dental Infections will remain an essential topic for both professionals and the public. Dental Infections represent a complex intersection of biology, treatment philosophy, and public health. Antibiotics play a role, but not the role many assume. Scientific evidence increasingly shows that Dental Infections require thoughtful evaluation rather than automatic antibiotic use. By examining bacterial behavior, resistance patterns, and clinical research, it becomes clear that antibiotics are tools, not universal answers, in the context of Dental Infections. A deeper understanding empowers better questions, more informed decisions, and a clearer perspective on oral health. ClinicHI continues to support informed discussions around Dental Infections, emphasizing knowledge, research, and long term awareness over quick assumptions.Get Your Free Consultation
Have questions? Leave your details and we'll get back to you as soon as possible.
Get Free Consultation