A Cavity is one of the most commonly discussed topics in oral health, yet it often remains misunderstood until discomfort appears. Many people assume a Cavity is only present when pain starts, but the reality is more complex and far more subtle. In its earliest stages, a Cavity can develop silently, influenced by daily habits, biological factors, and microscopic changes on the tooth surface.
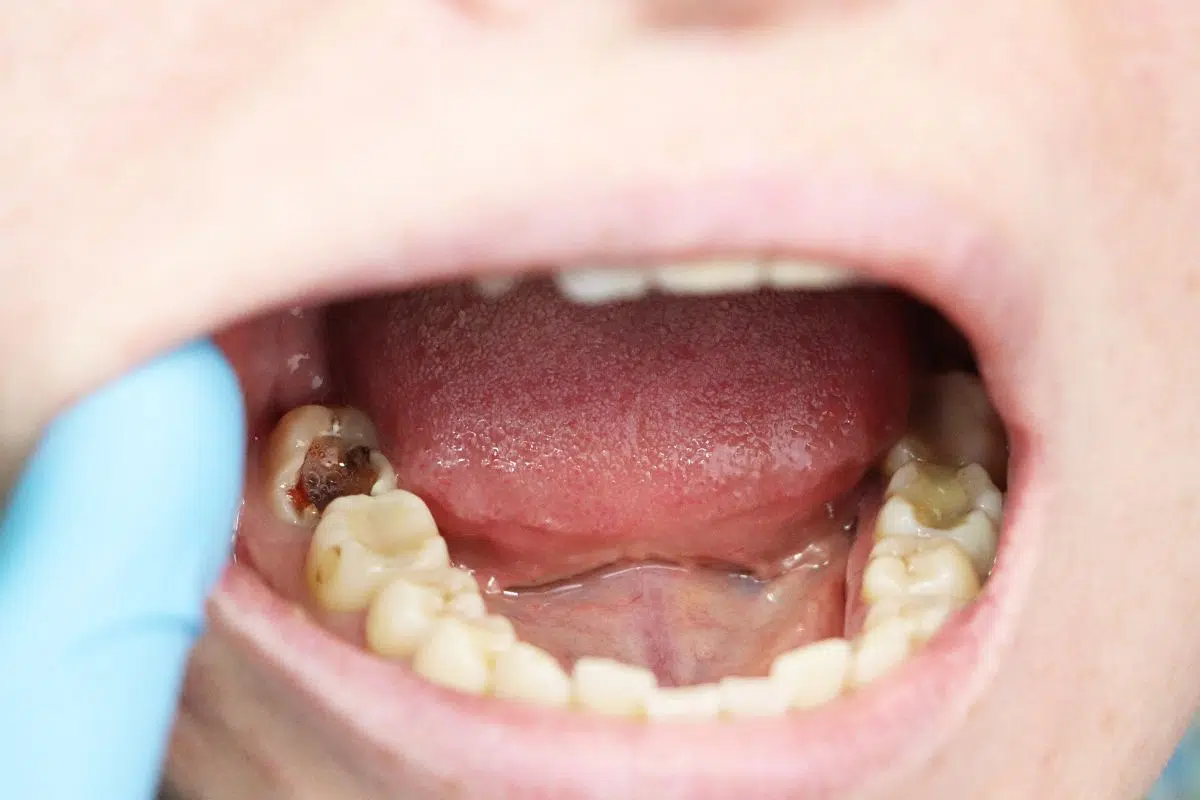
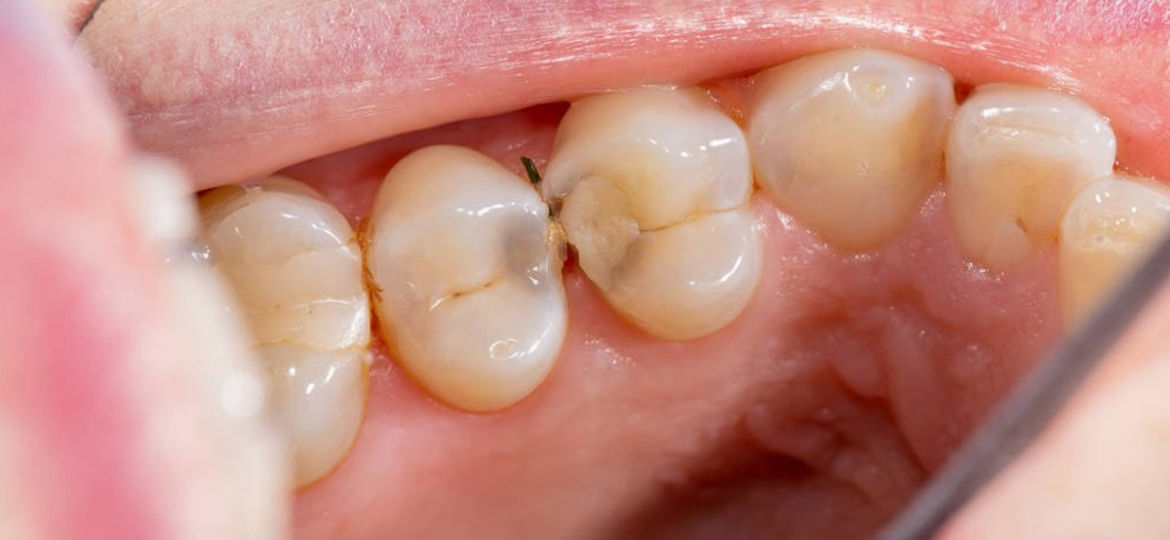
These observations form the backbone of how science understands Cavity prevention without offering direct health advice.

Understanding What a Cavity Really Is
A Cavity is not a sudden hole that appears overnight. Scientifically, it refers to the gradual breakdown of tooth enamel caused by acid producing bacteria. These bacteria feed on fermentable carbohydrates and produce acids that slowly dissolve mineral content from the tooth surface. From a research perspective, a Cavity is better understood as a dynamic process rather than a fixed condition. Early mineral loss can sometimes stabilize or progress depending on environmental factors. This explains why two people with similar habits may experience very different Cavity patterns over time. Interestingly, studies suggest that saliva composition, enamel density, and even genetics influence how easily a Cavity can develop. This makes the topic far more layered than a simple brushing frequency discussion.Early Signs of a Cavity You Might Overlook
The early stage of a Cavity rarely announces itself loudly. Instead, it often shows subtle signals that are easy to ignore or misinterpret. These early signs are not always painful, which is why awareness matters. Common early indicators linked to Cavity formation include:- Chalky white spots on the tooth surface
- Slight color changes that appear dull rather than shiny
- Brief sensitivity to temperature changes
- A rough feeling when the tongue passes over a tooth
Why a Cavity Does Not Always Hurt at First
Pain is commonly associated with a Cavity, but scientific findings show that discomfort usually appears later. Enamel itself has no nerves, so early enamel damage does not trigger pain signals. A Cavity becomes noticeable when it reaches dentin, the layer beneath enamel. Dentin contains microscopic tubules connected to nerve endings. Once acids penetrate this layer, sensations become more pronounced. This explains why many people are surprised when they learn they have a Cavity despite feeling fine. Pain is not an early warning system but rather a late stage indicator, according to most dental research models.How Daily Habits Influence Cavity Development
Daily routines play a central role in whether a Cavity develops or stalls. However, it is not only about sugar intake. Frequency, timing, and oral environment all matter. Scientific observations highlight that repeated acid attacks throughout the day are more influential than total sugar quantity. Each exposure lowers oral pH, giving a Cavity more opportunity to progress. Key habit related factors linked to Cavity risk include:- Frequent snacking on carbohydrates
- Reduced saliva flow during sleep
- Sticky foods that adhere to enamel
- Inconsistent oral hygiene timing
The Role of Oral Bacteria in a Cavity Process
Bacteria are essential players in every Cavity discussion. Certain strains, such as Streptococcus mutans, are strongly associated with acid production and enamel breakdown. What makes a Cavity particularly interesting from a scientific angle is that bacteria alone are not enough. They require fuel, time, and a favorable environment. Without these elements, even high bacterial levels may not cause significant damage. Research increasingly focuses on bacterial balance rather than elimination. A stable oral microbiome may reduce the likelihood that a Cavity progresses aggressively, offering a more nuanced understanding of prevention.Can a Cavity Stop or Slow Down Naturally?
One of the most debated topics in dental research is whether a Cavity can stop progressing. Evidence suggests that early enamel lesions may stabilize under certain conditions. Remineralization is a natural process where minerals are redeposited into enamel. Saliva plays a central role here. When conditions favor mineral return, the Cavity process may pause or remain unchanged for long periods. However, once structural damage occurs, the Cavity becomes less predictable. This distinction between early and advanced stages is a key theme in modern dental literature and highlights why early awareness matters.
Scientific Insights Into Cavity Prevention Patterns
Rather than offering instructions, scientific studies analyze patterns that correlate with lower Cavity incidence. These patterns are observational, not prescriptive. Researchers often note associations between Cavity rates and factors such as fluoride exposure, saliva quality, and dietary structure. Community level studies also show differences based on water mineral content and access to oral health education. A simplified overview of factors often discussed in research is shown below:| Factor Observed | Relation to Cavity Trends |
| Saliva flow rate | Lower rates linked to higher cavity activity |
| Enamel density | Denser enamel shows slower cavity progression |
| Meal frequency | Frequent intake increases cavity risk |
| Oral pH balance | Stable pH reduces cavity formation |
How Dentists Identify a Cavity Beyond Visual Checks
A Cavity is not always visible to the naked eye. Modern diagnostic methods rely on pattern recognition rather than simple inspection. Tools such as radiographic imaging and light based detection help identify changes in enamel density. These methods allow professionals to observe a Cavity before it becomes clinically obvious. This explains why routine evaluations are frequently mentioned in academic discussions about Cavity management. Early identification supports better understanding of how lesions evolve over time.The Bigger Picture: Why Cavity Awareness Matters
Understanding a Cavity is not about fear or urgency. It is about awareness. Dental science increasingly frames oral health as a continuum rather than a pass or fail condition. A Cavity reflects interactions between biology, behavior, and environment. By learning how it develops and what early signs look like, individuals gain context rather than anxiety. ClinicHI approaches this topic as an educational resource, aiming to explain the science behind a Cavity in a way that feels both reliable and engaging. Awareness leads to better questions, and better questions lead to more informed decisions.Get Your Free Consultation
Have questions? Leave your details and we'll get back to you as soon as possible.
Get Free Consultation