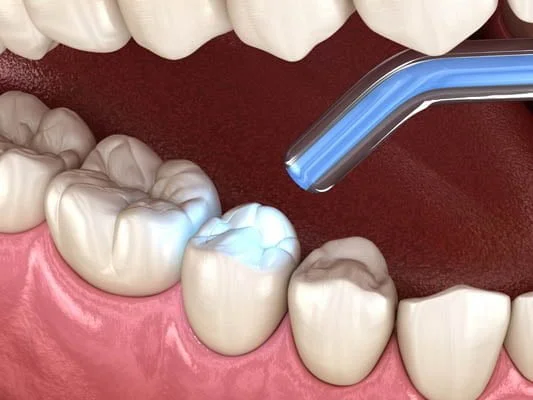
Dental fillings are one of the most common restorative treatments in dentistry, designed to repair decayed or damaged teeth. While the vast majority of patients tolerate these materials without issue, some individuals may develop sensitivities or allergic reactions to certain components. Understanding the mechanisms behind these reactions is crucial, as it informs both patient safety and clinical decision-making. Allergic responses to dental materials, though rare, are documented in dental literature and can range from mild oral irritation to more pronounced systemic symptoms.
Dental materials, including amalgam, composite resins, gold alloys, and ceramic fillings, contain various metals, polymers, and additives. Allergic reactions often involve the immune system identifying these substances as foreign, triggering responses such as inflammation or dermatitis. Research in oral immunology emphasizes that true hypersensitivity to dental fillings is uncommon but should not be overlooked, especially in patients with known allergies to metals or chemicals.
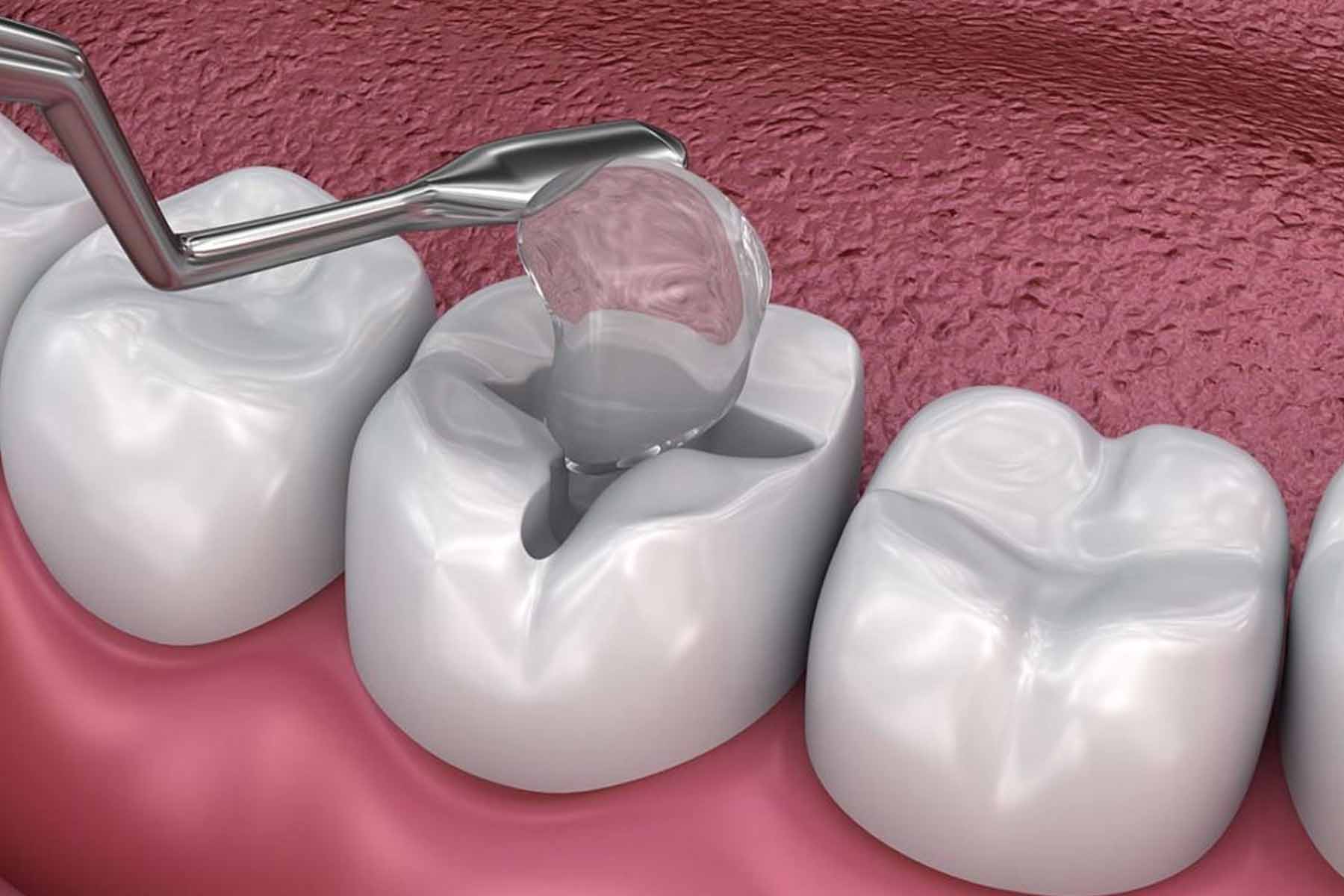
This comparative analysis helps both clinicians and patients weigh the benefits and risks of various dental fillings, emphasizing safety without compromising oral function.
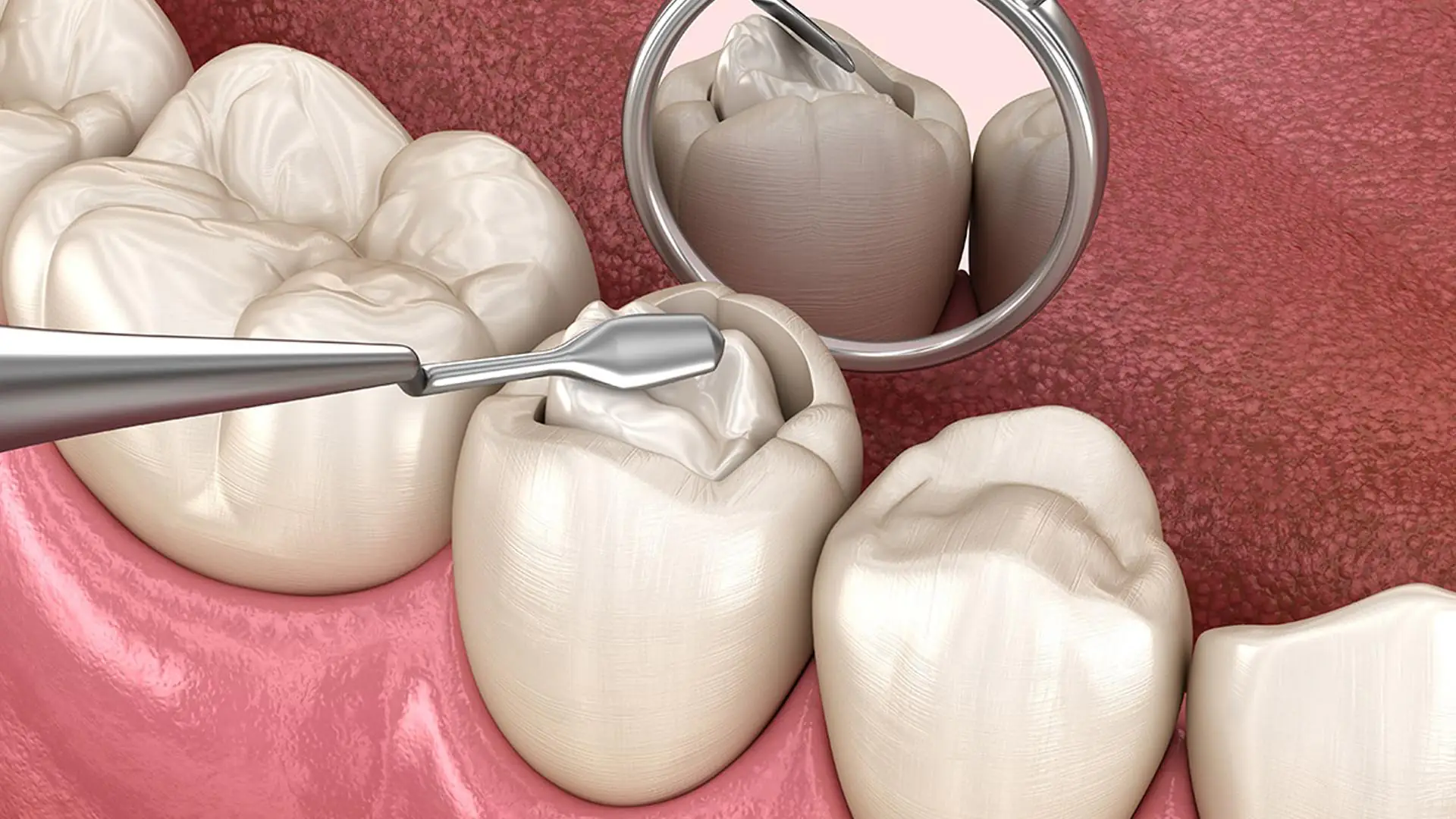

Types of Materials Used in Dental Fillings
Dental fillings can be classified based on their material composition. Amalgam fillings, composed primarily of mercury, silver, tin, and copper, have been used for over a century. Composite resins, on the other hand, are tooth-colored materials consisting of resin matrices and inorganic fillers. Gold and ceramic fillings provide alternative options for patients seeking durability and biocompatibility. Each material carries its own potential allergenic profile. For instance, mercury in amalgam can occasionally trigger immune reactions, while resin monomers in composite fillings have been associated with contact dermatitis in susceptible individuals. Studies in dental materials science highlight that selecting the appropriate filling material requires balancing mechanical performance, aesthetic considerations, and patient-specific sensitivities.Symptoms of Allergic Reactions to Dental Fillings
Allergic reactions to dental fillings can manifest in a variety of ways. Oral signs include localized swelling, redness, itching, and discomfort around the affected tooth. Some patients report a metallic taste, burning sensations, or recurrent mouth ulcers that persist despite standard oral hygiene measures. Systemic reactions, though less common, may present as skin rashes, hives, or generalized itching. Rarely, individuals with severe hypersensitivity may experience respiratory symptoms or exacerbation of preexisting conditions such as asthma. Clinical case studies underscore the importance of differentiating true allergic reactions from mechanical irritation or secondary infection, as symptoms can overlap.Diagnosis and Testing for Dental Filling Allergies
Diagnosing an allergy to dental fillings requires a careful combination of patient history, clinical examination, and sometimes specialized testing. Patch testing, commonly used in dermatology, can identify contact sensitivities to metals and polymers present in filling materials. Blood tests measuring specific immunoglobulin responses may also provide insight into systemic reactions. Dental professionals emphasize that diagnosis must consider all potential confounding factors, including oral hygiene practices, existing dental restorations, and environmental exposures. Documented case reports indicate that proper testing can prevent unnecessary removal of fillings while ensuring patient safety, highlighting the importance of evidence-based approaches in allergy management.Management and Alternative Materials
For patients confirmed to have an allergy to traditional dental materials, management strategies focus on replacing or avoiding the offending substance. Composite resins with hypoallergenic formulations, ceramic inlays, and gold fillings are often recommended alternatives. Treatment planning should integrate patient history, allergy testing, and aesthetic preferences. Clinicians may also employ temporary protective barriers or desensitization strategies for mild reactions. Literature in restorative dentistry supports that individualized approaches minimize risk while maintaining oral function and cosmetic outcomes.Preventive Measures and Clinical Recommendations
Preventing allergic reactions begins with comprehensive patient evaluation. Dentists are advised to obtain detailed medical and allergy histories before performing restorative procedures. Educating patients about potential symptoms and monitoring their response post-treatment is equally important. Moreover, ongoing research in biomaterials aims to develop fillings with enhanced biocompatibility and reduced allergenic potential. Scientific reviews suggest that innovation in resin chemistry, metal alloys, and ceramic technologies can significantly reduce the prevalence of adverse reactions, making dental fillings safer for a broader patient population.Understanding the Rare Possibility of Allergies
While most patients tolerate dental fillings without complications, a small subset may experience allergic or hypersensitivity reactions. Recognizing symptoms, conducting appropriate testing, and selecting alternative materials are key components of effective management. For patients concerned about allergies, consulting with a dentist knowledgeable in biomaterials and immunological responses ensures both safety and satisfaction. By integrating clinical expertise with current scientific understanding, dental care can remain both effective and personalized, addressing the rare but important phenomenon of filling-related hypersensitivity.Types of Allergic Reactions
Allergic reactions to dental fillings vary depending on the material and individual sensitivity. Localized oral reactions include redness, swelling, and persistent irritation around the treated tooth. Some patients experience a metallic taste or burning sensation that does not resolve with regular dental hygiene. Systemic reactions, although less frequent, may present as rashes, hives, or generalized itching. Rare cases involve respiratory symptoms or exacerbation of preexisting conditions like asthma. Understanding the spectrum of reactions helps dental professionals differentiate true allergies from mechanical irritation or secondary infections.Diagnosis Methods for Dental Filling Allergies
Accurate diagnosis of dental filling allergies requires a combination of patient history, clinical examination, and testing. Patch tests are commonly used to detect contact hypersensitivity to metals or resin components. Blood tests may also identify specific immunoglobulin responses linked to systemic reactions. Proper diagnosis prevents unnecessary removal of fillings while ensuring patient safety. Studies indicate that integrating clinical evaluation with laboratory tests provides a reliable approach to identifying true allergic reactions in patients with suspected sensitivities.Hypoallergenic and Alternative Materials
For patients with confirmed allergies, choosing suitable dental filling materials is crucial. Options include ceramic inlays, gold restorations, and hypoallergenic composite resins. These alternatives reduce the risk of immune responses while maintaining functionality and aesthetic appeal. Dentists often tailor material selection based on patient history, severity of reactions, and cosmetic needs. Research in restorative dentistry highlights the importance of individualized strategies to prevent adverse outcomes and ensure long-term oral health.Management Strategies and Symptom Relief
Managing dental filling allergies involves both preventive and reactive approaches. Mild reactions may be alleviated with topical treatments or temporary desensitization, while severe reactions may necessitate replacement of the allergenic filling. Patient education is critical for monitoring symptoms, avoiding triggers, and understanding treatment options. Evidence suggests that proactive management minimizes discomfort, enhances patient confidence, and preserves overall oral function.Long-Term Monitoring and Follow-Up
Patients with known sensitivities to dental fillings benefit from ongoing monitoring. Regular dental check-ups allow clinicians to detect early signs of adverse reactions and address them promptly. Scientific literature emphasizes that continuous follow-up, combined with patient awareness, ensures safety and contributes to better clinical outcomes. Long-term management strategies support both oral health and patient satisfaction, particularly for those with heightened allergenic risks.Emerging Research in Dental Material Biocompatibility
Recent studies in dental material science focus on enhancing biocompatibility and reducing allergenic potential. Innovations in resin chemistry, ceramic composites, and metal alloys aim to minimize immune responses while maintaining durability and aesthetics. Ongoing research indicates that patients with previous sensitivities can safely receive advanced restorative treatments with lower risk. Integration of these findings into clinical practice represents a significant step toward personalized and safe dental care for all patients.Case Studies Highlighting Dental Filling Allergies
Case studies provide insight into the variability and impact of dental fillings allergies. In one documented case, a patient experienced persistent oral irritation and localized swelling after receiving a composite resin filling. Patch testing confirmed a hypersensitivity to the resin’s chemical components. Following replacement with a hypoallergenic ceramic inlay, symptoms resolved completely within weeks. Another case involved a patient with a history of metal sensitivities who developed a rash and itching after a gold alloy filling. Removal and replacement with a biocompatible composite eliminated the reaction, demonstrating the importance of individualized material selection based on allergy history. These examples underscore how proper diagnosis and material choice can prevent long-term discomfort and complications.Comparative Table: Common Filling Materials and Allergenic Potential
| Material Type | Allergenic Risk | Longevity | Notes |
| Amalgam (Silver) | Moderate | High | Contains mercury; rare hypersensitivity |
| Composite Resin | Low to Moderate | Moderate | May contain BPA derivatives; patch testing advised |
| Ceramic/Inlays | Very Low | High | Hypoallergenic, highly aesthetic |
| Gold Alloy | Low | High | Rare allergic reactions; excellent durability |
Patient Experiences and Quality of Life
Patients with dental fillings allergies often report significant improvements in quality of life after switching to hypoallergenic alternatives. Beyond symptom relief, many describe reduced anxiety about future dental procedures and enhanced confidence in eating and speaking comfortably. Psychological well-being plays a crucial role, as untreated allergic reactions may contribute to chronic stress, sleep disturbances, or avoidance of dental care. Research highlights that patient-centered management, which includes education, symptom tracking, and follow-up visits, not only addresses physical reactions but also supports overall mental health. This reinforces the need for a comprehensive approach to allergy management in dentistry.
Preventive Measures and Clinical Guidelines
Preventing allergic reactions to dental fillings involves pre-procedural assessment and proactive planning. Dentists may use detailed medical histories, allergy questionnaires, and selective testing to identify patients at risk. For known sensitivities, material substitution or staged treatments can mitigate adverse outcomes. Clinical guidelines recommend ongoing patient monitoring, documentation of reactions, and communication between dental and medical providers. Preventive strategies reduce emergency interventions and optimize both functional and aesthetic outcomes for patients with potential allergies.Emerging Technologies and Future Directions
Advancements in dental materials science are reshaping approaches to dental fillings allergies. New biocompatible composites, metal-free restorations, and nanotechnology-based ceramics aim to minimize immune responses while improving durability and aesthetics. Future directions include personalized dentistry using genetic and immunologic profiling to predict sensitivities before treatment. This proactive approach could revolutionize patient care, offering safer, longer-lasting, and more comfortable restorative options tailored to individual immune profiles.Summary and Practical Takeaways
In conclusion, dental fillings can provoke allergic reactions, though the prevalence is relatively low. Identifying at-risk individuals, using hypoallergenic materials, and following evidence-based management protocols ensures safety and patient satisfaction. Regular monitoring, patient education, and incorporation of emerging materials provide a comprehensive framework for preventing and addressing allergic responses.Get Your Free Consultation
Have questions? Leave your details and we'll get back to you as soon as possible.
Get Free Consultation